
CMRR
Center for Magnetic Resonance Research, Department of Radiology
Research Highlights
You are here
Deep Brain Stimulation
Direct visualization of surgical DBS targets using high-field (7 Tesla) MRI
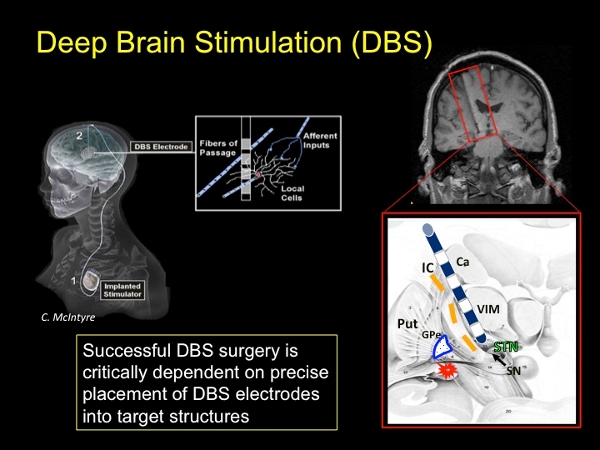
Deep brain stimulation (DBS) surgery is used for treating movement disorders, including Parkinson’s disease, essential tremor, and dystonia. Successful DBS surgery is critically dependent on precise placement of DBS electrodes into target structures. Current clinical imaging methods (1.5 Tesla MRI) have insufficient resolution to delineate the targets of DBS surgery. Recent advances in MRI technology and stronger magnets (7 Tesla) have allowed for superior image resolution.
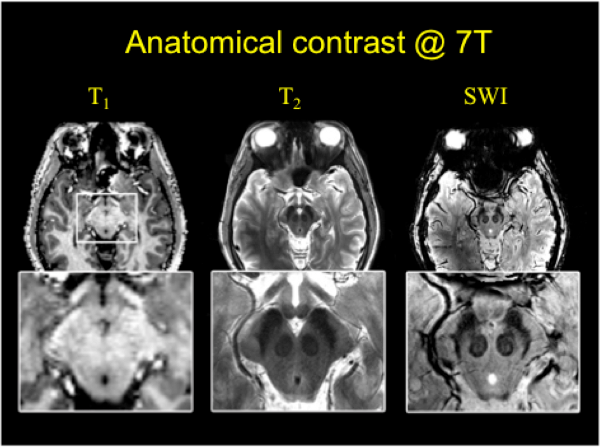
Superior image resolution and contrast obtained at 7T in vivo, using susceptibility-weighted imaging, dramatically improved anatomical delineation of DBS targets and allowed for identification of internal architecture within these targets. (Abosch et al.,Neurosurgery 2010)
In-vivo visualization of the human basal ganglia and their structural connectivity
 |
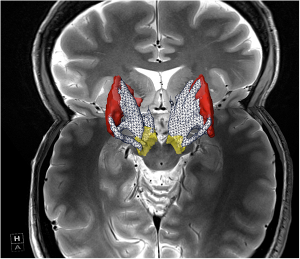 |
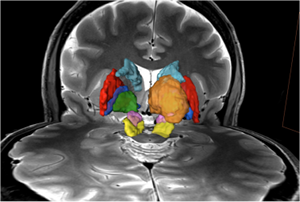
Taking advantage of increased contrast attainable at 7T, it is possible to visualize and deliniate subcortical nuclei in much greater detail, such as the subthalamic nuclei (STN) that is not seen clearly or not at all at lower magnetic fields. The 3D models created in this way (left panel depicts the different structures as color coded volumetric renditions) are used to examine connectivity among these subcortical nuclei by constructing 3D models of white matter tracts from data obtained with high angular resolution diffusion imaging (HARDI). Diffusion imaging is increasingly being used clinically to localize white matter lesions that do not show up on other forms of clinical MR imaging. (Lenglet et al., 2012)
REFERENCES
An assessment of current brain targets for deep brain stimulation surgery with susceptibility-weighted imaging at 7 tesla. Abosch A, Yacoub E, Ugurbil K, Harel N. Neurosurgery. 2010 Dec;67(6):1745-56;
Comprehensive in vivo mapping of the human basal ganglia and thalamic connectome in individuals using 7T MRI. Lenglet C, Abosch A, Yacoub E, De Martino F, Sapiro G, Harel N. PLoS One. 2012;7(1):e29153